Maternal and Infant Health
A 2020 report by the Centers for Medicare & Medicaid Services (CMS) notes that in an ideal maternal health system, all people would have access to comprehensive, seamless medical and behavioral health care as well as economic and social supports. Additionally, they would be engaged with this system before, during and after pregnancy, and care would be available in places more proximate than a hospital. The majority of women in the U.S. do not receive this type of care.
For most Americans, access to health care starts with health insurance. Health care coverage before and after pregnancy is associated with better health outcomes for both mother and infant. One example is coverage for prenatal care. Babies of mothers who do not get prenatal care are three times more likely to have a low birth weight and five times more likely to die than those born to mothers who do get care. With the implementation of the Affordable Care Act (ACA), health insurance coverage expanded dramatically for most citizens of the U.S. However, there is more that states can do to ensure that prenatal, delivery and postpartum care are available to women through a comprehensive insurance coverage plan.
Health insurance coverage should include support for perinatal mental health and substance use disorders, from screening through treatment, to address the leading causes of maternal mortality. Coverage could also include postpartum care that extends beyond the traditional single visit six weeks postpartum. Slightly more than half (52 percent) of all deaths occur after the day of delivery through one year postpartum, while almost one-third (31 percent) occur during pregnancy.
Ultimately, it is critically important for both commercial and public health insurance to include robust perinatal coverage, especially behavioral health services and longer-term postpartum care. The ACA greatly improved coverage of maternity health services. In particular, 20 million people have gained coverage, financial assistance has become available to purchase coverage and the quality of coverage offered has been improved. But there are still significant differences among states in the prenatal, labor and delivery, and postpartum services covered. Specifically, the ACA requires small group and individual market plans to cover maternity and newborn care among the required essential health benefits (EHBs), but states are able to select a benchmark plan to define the specific services covered under each category which can serve to limit coverage. Similarly, there is a great deal of variation in services and outcomes offered through Medicaid. In 2021, 41 percent of births in the U.S. were financed by Medicaid. However, compared to women with private health insurance, women with Medicaid coverage were more likely to report: no postpartum visit, returning to work within two months of birth, less postpartum emotional and practical support at home, lack of decision autonomy during labor and delivery, being unfairly treated and disrespected by providers because of their insurance status and not exclusively breastfeeding at one week and six months.
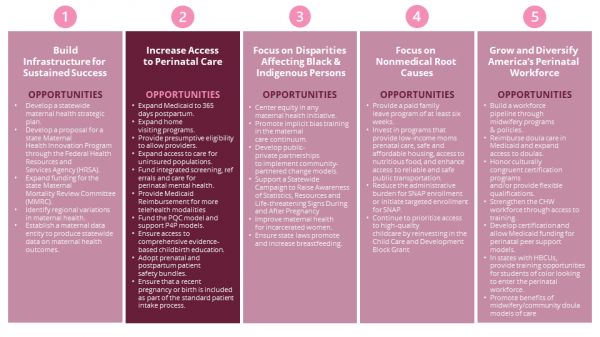 Opportunity 6: EXPAND MEDICAID TO 365 DAYS POSTPARTUM.
Opportunity 6: EXPAND MEDICAID TO 365 DAYS POSTPARTUM. Extending Medicaid coverage through 12 months postpartum is crucial to addressing the current maternal health crisis. The first year after birth is a significant period, as more than half of pregnancy-related deaths happen during this time. Extending coverage can help new mothers overcome barriers to physical and mental health care, improve health outcomes and potentially reduce disparities. Approximately 65 percent of births by Black mothers are covered by Medicaid, so extending the postpartum coverage would positively impact outcomes and reduce disparities.
Currently, the default for Medicaid coverage ends 60 days after birth, but through Section 9812 of the 2021 American Rescue Plan Act states have the option of extending Medicaid 12 months postpartum through a less cumbersome administrative processes, as well as drawing on more federal matching funds.79F[iii] The American College of Gynecology guidance notes that the postpartum period should be an ongoing process “with services and support tailored to each woman’s individual needs.” This may include physical recovery from birth, an assessment of social and psychological well-being, chronic disease management and initiation of contraception, among other services. Under the Consolidated Appropriations Act of 2023, the extension option for Medicaid postpartum coverage has been made permanent. Therefore, once states choose to extend, they will continue to receive federal matching funds.
State Spotlight: As of June 2023, 35 states have extended their postpartum coverage through a full year postpartum. Louisiana was a national leader in extending postpartum coverage. The Centers for Medicare Services approved the state’s plan amendment in April 2022. States have approached this through combinations of federal action, state plan amendments or waivers, and laws or bills.
Opportunity 7: EXPAND EVIDENCE-BASED HOME VISITING PROGRAMS.Home visiting is a prevention strategy designed to support pregnant families, promote infant and child health, foster child development and school readiness, and help prevent child abuse and neglect. Home visiting programs are voluntary and offer vital support to parents as they manage the challenges of raising babies and young children.
States are covering these evidence-based services, such as home visiting during the perinatal period, to improve continuity of care for pregnant and postpartum people enrolled in the Medicaid Children’s Health Insurance Program (CHIP). States leverage other federal, state, local and private funding sources to finance these services and in some cases use existing Medicaid services to cover components of home visiting.
One example of a robust universal home visiting model is Family Connects, which is part of a clearinghouse of highly effective approaches. Family Connects demonstrates improvements in child health, linkages and referrals, maternal health and positive parenting practices. It consists of one to three nurse home visits, typically when the infant is two to 12 weeks old, and follow-up contacts with families and community agencies to confirm families’ successful linkages with community resources. During the initial home visit, a nurse conducts a physical health assessment of the mother and newborn, screens families for potential risk factors and may offer direct assistance, such as guidance on infant feeding and sleeping. If a family has a significant risk or need, the nurse connects the family to community resources. Family Connects is currently implemented in 12 states.
State Spotlight: In 2019, Kansas served an estimated 23.8 percent of children under age three in families with incomes of less than 150 percent of the Federal Poverty Level in the state’s home visiting programs. As of 2021, families in the state have access to five out of a possible seven evidence-based program models that have a demonstrated impact on parenting and are designed for families with young children. In 2021, Maryland launched a maternal and child health care transformation initiative to fund the expansion of current maternal health-focused programs, which includes home visiting services. In Michigan, the statewide Maternal Infant Health Program serves over 20,000 Medicaid-eligible families, with prenatal and postnatal home visiting covered. Michigan is creating more awareness of their Home Visiting Program and other state maternal health programs by developing a mobile pregnancy app to connect users to state maternal health programs. In 2021, New Jersey joined Oregon in enacting Universal Newborn Nurse Home Visiting enabling all new moms, including those that experience a stillbirth and those that adopt, to receive up to three visits by a registered nurse in their home. Additional states with robust home visiting programs include Iowa and Maine.
Opportunity 8: PROVIDE PRESUMPTIVE ELIGIBILITY TO ALLOW PROVIDERS TO TREAT PREGNANT PEOPLE WHEN THEY FIRST SEEK PRENATAL CARE RATHER THAN WAITING UNTIL AFTER MEDICAID ELIGIBILITY IS REVIEWED AND DETERMINED.Despite being eligible for Medicaid coverage, it often takes pregnant women days or sometimes weeks to acquire Medicaid, delaying their prenatal care and treatment. Presumptive eligibility is a policy that allows health care providers to provide temporary Medicaid or CHIP coverage to individuals who are likely to qualify for these programs but have not yet completed the application process.
State Spotlight: As of 2020, 30 states, offer presumptive eligibility for pregnant women. Express Lane Eligibility (ELE) is another policy that could increase access to Medicaid services for eligible women while also streamlining the application process. ELE allows state Medicaid or CHIP programs to rely on the application findings from other state programs, such as Head Start or the Supplemental Nutrition Assistance Program (SNAP), to offer health care services. As of 2021, ELE is offered in Alabama, Colorado, Iowa, Louisiana, Massachusetts, South Carolina and South Dakota.
Opportunity 9: EXPAND ACCESS TO MATERNAL AND INFANT CARE FOR UNINSURED POPULATIONS.Lawfully present immigrants may qualify for Medicaid and CHIP but are subject to certain eligibility restrictions. In general, lawfully present immigrants, including most lawful permanent residents or green-card holders, must have a “qualified” immigration status to be eligible for Medicaid or CHIP and must wait five years after obtaining qualified status before they may enroll. Noncitizens, including lawfully present and undocumented immigrants, are significantly more likely to be uninsured than citizens. Medicaid expansion to households with 200 percent of the federal poverty level, allowing Deferred Action for Childhood Arrivals (DACA) eligible immigrants to receive CHIP prenatal services and reducing the five-year Medicaid eligibility waiting period for immigrants can cover these gaps in care during the perinatal period.
State Spotlight: In 2021, Oregon implemented the Cover All People legislation as part of House Bill 3352 to include low-income, undocumented adults in the Oregon Health Plan. As of July 2022, there is $100 million in state funding for the expansion. In July 2022, Illinois lowered the age for Medicaid eligibility for residents regardless of citizenship to 42 years old through authorization from the Illinois General Assembly.
Opportunity 10: FUND AND PRIORITIZE INTEGRATED SCREENING, REFERRALS AND CARE FOR PERINATAL MOOD AND ANXIETY DISORDERS (PMADS), PERINATAL SUBSTANCE USE DISORDERS (SUDS) AND INTIMATE PARTNER VIOLENCE (IPV).As the most common complications in pregnancy, PMADs, SUDs and IPV are distinct yet often intertwined, and associated with a range of adverse outcomes for pregnant persons and their families. Some estimates indicate that 15.9 percent of pregnant people in the United States smoked cigarettes, while 8.5 percent consumed alcohol and 5.9 percent used illicit drugs. IPV can result in insufficient or inconsistent prenatal care, poor nutrition, inadequate weight gain, substance use and increased prevalence of depression, as well as adverse neonatal outcomes, such as low birth weight and preterm birth and maternal and neonatal death.
Routine screenings, interventions and referrals through an integrated care model for mothers and their families are essential. Markers of strong, integrated care include: training health care providers to identify mental health, substance use and IPV issues for pregnant and postpartum women, early and periodic screening that supports both identification and stigma reduction through frequent conversations with families, accessing treatment across the continuum of mild to severe issues, and working with pediatric providers to screen and support mothers and families with mental health and substance use disorders throughout the first year of well-child visits.
State Spotlight: Alabama expanded Medicaid to include screening, brief intervention and referral to treatment for early intervention and treatment of SUDs. In 2021, Louisiana began allowing separate Medicaid reimbursement for perinatal depression screenings of an enrolled caregiver during a well-child visit from birth to 365 days postpartum. In New Mexico, pregnant women of color reported receiving discriminatory substance use treatment and screening, so the New Mexico Children, Youth and Families Department (CYFD) and the Department of Health (DOH) created systemic training for hospital staff to provide less stigmatizing treatment. Further, the Children’s Code was amended through House Bill 230 so that substance use during pregnancy is not singular grounds for a mandatory child abuse report. New Mexico’s amendment to the Children’s Code included a Plan of Safe Care in which families affected by substance use make a plan during pregnancy with a multidisciplinary team to ensure the health of infants and mothers. Plans of Safe Care include the following four components for care and support during the perinatal period: physical health, behavioral health to address substance use, infant health and development and parenting/family support to connect the family with social services. Currently, 33 states have Plans of Safe Care to address the needs of infants and mothers.
Opportunity 11: PROVIDE MEDICAID REIMBURSEMENT FOR MORE TELEHEALTH MODALITIES, INCLUDING LIVE VIDEO, STORE-AND-FORWARD, REMOTE PATIENT MONITORING, TELE-ULTRASOUND, REMOTE NONSTRESS TEST AND EMAIL/PHONE/FAX.With the national increase in maternal care deserts, people across the country are being forced to travel further for perinatal care. Adoption of Medicaid reimbursement policies and ensuring that codes for these procedures allow, or even specify, that the activity can take place in the home is important because it allows patients to be monitored and cared for without the cost and burden of frequent prenatal visits.
Two U.S.-based studies investigated a combination of telehealth visits and reduced in-person visits for prenatal care to determine the feasibility of telehealth maternal care. The two studies demonstrated that telehealth resulted in higher satisfaction and lower prenatal stress for patients compared with those receiving in-person care. It is necessary to note that telehealth can only be effective if access to technology is universal.
State Spotlight: The Extension for Community Healthcare Outcomes, Project ECHO, is a tele- mentoring approach that brings expertise to patients in medically underserved areas by connecting specialty physicians to primary care physicians. Project ECHO, which began in New Mexico, is now one of the many maternal telehealth policies in Virginia aimed at improving health coverage and supporting the alignment of reimbursement for telehealth services across patients. In Georgia, the Healthy Babies Act was passed in 2023 to pilot a two-year maternal telehealth program for Medicaid enrollees that provides access to remote patient monitoring, remote fetal nonstress tests and tele-ultrasound. In Missouri, the Medicaid Department issued guidance clarifying that the home can be a place of service for the fetal non-stress test. In Oklahoma, expanding telehealth services for birthing women and infants is part of the Oklahoma Maternal Health Task Force 2020-2024 Strategy.
Opportunity 12: FUND THE STATE’S PERINATAL QUALITY COLLABORATIVE (PQC) TO INCREASE CAPACITY AND SUPPORT PAY-FOR-PERFORMANCE MODELS.Nearly every state already has or is developing a PQC, which supports hospitals and clinicians to engage with quality improvement tools. PQCs have made population health improvements by improving breastfeeding rates, reducing elective deliveries without a medical indication before 39 weeks’ gestation, reducing unnecessary cesarean births among low-risk pregnant women, reducing health care setting-associated infections in newborns, bringing down rates of hemorrhage and hypertension and reducing rates of preterm births.
About half of states monitor or report state-level metrics related to maternal health. While most states require managed care organizations to report maternity-related quality measures to the state, few use performance improvement measures. Quality improvement tools may be more widely used by incorporating pay-for-performance models or by adopting existing perinatal risk assessment tools. There is a need to invest more resources into PQCs and provide capacity support to expand the impact of their work.
State Spotlight: To address rising maternal deaths associated with preeclampsia, Illinois’ PQC conducted a program to improve care for pregnant and postpartum women with severe preeclampsia and eclampsia in 112 hospitals. The number of women receiving medication within 60 minutes increased from 42 percent to 85 percent during the program, and the rate of severe pregnancy complications among pregnant women experiencing hypertension at delivery decreased by 41 percent.
Opportunity 13: ENSURE ACCESS TO COMPREHENSIVE EVIDENCE-BASED CHILDBIRTH EDUCATION FOR ALL MEDICAID BENEFICIARIES AS PART OF STANDARD PRENATAL CARE.Childbirth education (CBE) is designed to help pregnant women and their support unit manage the physical, emotional and psychological changes during the perinatal period, increase their knowledge and access to community resources, improve their ability to advocate for care and increase the likelihood of positive birth outcomes. CBE is also a recommended strategy for cesarean rate reduction.
States can work with their perinatal quality collaborative to align hospital practices and philosophies with evidence-based childbirth education; assess and mitigate barriers to childbirth education; include flexible educational formats, such as interactive web-based learning; and implement prenatal care models that efficiently integrate comprehensive pregnancy and childbirth education into routine visits, such as group prenatal care.
State Spotlight: Washington’s Medicaid program offers pregnant women a series of educational group sessions with at least six hours of instruction, led by a trained educator who has both a certification or credentials from a training organization that meets the Childbirth Educator training standards set by the International Childbirth Education Association (ICEA) and a current Core Provider Agreement and National Provider Identifier (NPI), to prepare each pregnant woman and her support person(s) for labor and delivery. In Wisconsin, CBE is covered through Medicaid if a pregnant person is both at higher risk for adverse outcomes and are also enrolled in the state’s Prenatal Care Coordination program.
Opportunity 14: IMPLEMENT PRENATAL AND POSTPARTUM PATIENT SAFETY BUNDLES TO ADDRESS ONGOING QUALITY IMPROVEMENT.Patient safety bundles are a structured way of improving the processes of patient care.108F[i] The Alliance for Innovation on Maternal Health (AIM) is a quality improvement initiative to support best practices that make birth safer, improve maternal health outcomes and save lives by implementing best practices in hospitals. AIM developed eight bundles that include actionable steps that can be adapted to a variety of facilities and resource levels to address the leading causes of preventable maternal mortality.
State Spotlight: In Texas, the Department of State Health Services (DSHS) teamed up with AIM and the Texas Hospital Association to create the TexasAIM initiative to help hospitals and clinics carry out maternal safety projects. Currently, TexasAIM supports three AIM bundles such as the Obstetric Hemorrhage Bundle, the Obstetric Care for Women with Opioid Use Disorder Bundle and the Severe Hypertension in Pregnancy Bundle. The Texas DSHS connects any interested hospitals and clinics to resources, tools and the AIM data portal.
Opportunity 15: HOLD PROVIDERS ACCOUNTABLE FOR ENSURING THAT A RECENT PREGNANCY OR BIRTH IS INCLUDED AS PART OF THE STANDARD PATIENT INTAKE PROCESS.Maternal and infant health outcome improvement is challenged by the number of fragmented touchpoints in a health care system that exist from conception through one year postpartum. For example, a woman may shift from a midwife-led clinic to a hospital delivery with an OB-GYN provider, then go back to a primary care provider in the postpartum period, followed by another shift to having the majority of interactions with their child’s pediatrician. Encouraging connection and communication among this system of providers is another approach to ensuring accountability for high-quality care and outcomes.
State Spotlight: In 2020, New Jersey enacted bill A5031/S3455, which requires hospital emergency departments to ask people of childbearing age about any pregnancy in the past 365 days. This simple approach could lead to catching health issues exacerbated by a pregnancy-related condition a full year postpartum.
相关知识
Maternal and Infant Health
Prevalence and the correlation factors analysis of maternal morbidity for postpartum women
Pregnant women: addressing maternal mental health in Africa
China’s Actions to Achieve Universal Health Coverage for Children
Arts and health
基于机器学习的产妇健康与婴儿行为特征之间的关系建模。
impact on the recovery of health guidance on maternal puerperal(影响对孕产妇产后的恢复健康指导).doc
Newborns: improving survival and well
Landscape Analysis to Accelerate Actions to Improve Maternal and Child Nutrition In Namibia
母乳喂养与心理健康|Breastfeeding and Mental Health
网址: Maternal and Infant Health https://www.trfsz.com/newsview1706384.html
推荐资讯
- 1发朋友圈对老公彻底失望的心情 12775
- 2BMI体重指数计算公式是什么 11235
- 3补肾吃什么 补肾最佳食物推荐 11199
- 4性生活姿势有哪些 盘点夫妻性 10428
- 5BMI正常值范围一般是多少? 10137
- 6在线基础代谢率(BMR)计算 9652
- 7一边做饭一边躁狂怎么办 9138
- 8从出汗看健康 出汗透露你的健 9063
- 9早上怎么喝水最健康? 8613
- 10五大原因危害女性健康 如何保 7828






